Adrenal Fatigue and IBS, the Hidden Connection
The term ‘Adrenal Fatigue’ might have been thrown around a lot lately but that doesn’t mean the actual condition isn’t very real and very debilitating. While IBS-type symptoms let you know that your digestive system isn’t happy, the symptoms of Adrenal Fatigue make you feel like you are falling off a cliff. You are tired, completely worn out and can’t retain your usual energy levels, no matter what you do. Through my own journey, and those of my clients, with both Adrenal Fatigue and IBS, I’ve learnt a lot about the often overlooked connection between these two misunderstood conditions. So, bringing awareness to this is pretty close to my heart and something you need to know if you are suffering.
Me, (looking glamorous) on the Inca Trail heading up to ‘Dead Woman’s Pass’, feeling exactly as the name suggests. I don’t really recommend adventure hiking holidays while suffering from Adrenal Fatigue and IBS, digestive issues and a generally run-down immune system, but I had no idea what was going on with my body at the time. Photo credit: Jesse Lindemann
With that in mind, here’s what we’ll be covering:
> What is Adrenal Fatigue and what does it have to do with stress?
> Six warning signs that you may be suffering from Adrenal Fatigue
> The connection between Adrenal Fatigue and IBS
> How to get tested for both adrenal dysfunction and the underlying root cause
> How to reverse Adrenal Fatigue naturally
Adrenal fatigue is basically a collection of symptoms you get when the adrenal glands stop functioning as well as they should. And it all relates to cortisol, your body’s stress hormone. With so many stressors in our daily lives, as well as the stressors from activities we love, like travel and exercise, it’s not hard to see why Adrenal Fatigue is becoming a really common occurrence.
The three types of stress
Everyday we are bombarded with stressors from the moment we wake up to the moment we go to bed. These stressors come from three main sources:
1. Mental/emotional
2. Physical; or
3. Biochemical sources
For anyone with IBS, these biochemical stressors can be anything from food sensitivities or dietary triggers (FODMAPs, histamines, etc.) to pathogens like parasites, bacteria or yeast overgrowths.
But the key thing to note here is that the body responds to ALL types of stress in a similar way, whether it is a physical stressor such as a broken bone, a mental/emotional stressor such as a stressful day at work, or a hidden, internal stressor like a gut parasite mentioned above (1).
The HPA Axis and the stress response
HPA Axis Diagram Adrenal Fatigue IBS
Now for the science of how your body responds to all of that stress. This diagram is a simple illustration of the body’s physiological stress response. Once your brain has registered a threat (stress) - whether it’s mental, physical or biochemical, the hypothalamus and the pituitary glands start the release of Corticotropin-releasing hormone (CRH) and Adrenocorticotropic hormone (ACTH) to help react to the threat (the fight-or-flight response). This includes increased blood flow to the brain, heart and muscles. The adrenal glands then release cortisol, our stress hormone, to inhibit processes not necessary for immediate survival, like digestion and the immune system response amongst others. The response your body has to stress occurs via the hypothalamus-pituitary-adrenal (HPA) axis (2).
While inhibiting digestion and the immune system might be a useful response by the body to an ACUTE stress (e.g. being chased by a lion), it is not so useful when it’s a 24/7, 365 days a year kind of low-level CHRONIC stress (e.g. daily stress from family, work, environmental toxins and yes, gut infections and food sensitivities). It’s not hard to see why your poor adrenals get exhausted from pumping out the cortisol all day, every day, when they are only used to working under short-term and acute stress. It’s like Usain Bolt trying to sprint a marathon, eventually he is is going to run out of steam...
So what do we have so far: stress (of any kind) coming into the body, the HPA axis working and telling the body to put out cortisol (the stress hormone), turning off digestion and the immune system, then more stress coming in and more cortisol being put out as a continuing cycle. Unfortunately, this stressful cycle is all too normal because of the way we live and the stressors of modern life. Which means, when is our digestive and immune systems ever going to get a chance to work properly?
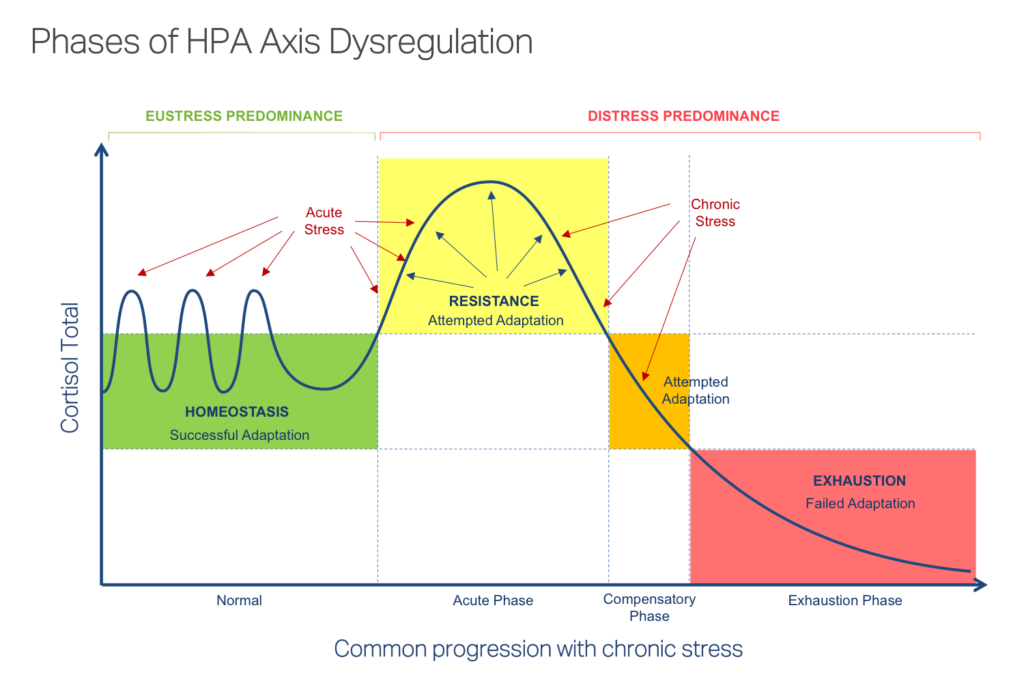
The three phases of cortisol dysregulation
A “normal” and healthy human’s body and adrenals like to achieve homeostasis – a state of balance within the body where stress is easily dealt with. If we get stressed by a work deadline, broken bone or gut pathogen and our cortisol levels rise, then once the acute stress is resolved, our cortisol levels return to normal. In homeostasis there is an appropriate amount of cortisol in the body at any given time.
There are three phases of Cortisol Dysregulation and they are a progression from bad to worse. They are as follows:
Acute phase: Initially, this phase represents a healthy human’s response to acute stress. The response of the adrenals is to produce cortisol, adrenalin and other hormones - a normal process known as allostasis (3). Adrenaline will also be produced with cortisol in response to the stress, and this usually makes you feel great and like you are managing stress really well. Genetics, as well as the type and duration of the stress, will impact how long you are able to maintain this high level of cortisol output (4). If the stress continues and becomes chronic, there will be a continual demand on the adrenals to push out high levels of cortisol. With ongoing stress, the body and adrenals get to a point where they don’t respond like they used to. The adrenals are worn out from all of the extra work they have been doing to manage the increased stress for months, or sometimes years. Now the acute stress state becomes a chronic stress state and the adrenals will reach a point where they are no longer able to adapt to high cortisol needs.
Cortisol is catabolic, meaning high levels during the acute phase breaks things (like body tissue) down (5). Your adrenal glands can’t keep this up forever, so at some point, despite the body’s continued need for cortisol, the production by the adrenal glands will start to decrease. And so begins the downward slide...
This is the point where cortisol begins to decline, even though the body is still under stress and needs high amounts of it. The body is now on the downwards slide and the person may start to notice some mild symptoms as cortisol diminishes and the adrenals and other organs, glands and systems lose homeostasis, or balance.
Compensatory phase: Progress from acute to compensatory phase continues as cortisol diminishes further, as result of the adrenals not working correctly. Here, cortisol levels fall within the “normal” range on a lab test, however we know it is not “normal” because you are under continued stress and your body is showing symptoms that it is not dealing with the stress correctly. Further breakdown is occurring in the body and symptoms are present from the continued loss of function. Here, people start to self-medicate with things like caffeine, foods and medicines to help get themselves through the day. This is what we refer to as Adrenal Fatigue. This is the phase that most of my clients find themselves in.
Exhaustion phase: Finally, cortisol drops below normal levels on a lab test and you enter into exhaustive phase. Here, you have further diminished function and either more severe or a greater number of symptoms. The adrenals are now “tanked” and you have reached a phase of failed adaptation where you will require medications to manage symptoms and disease, and potentially even surgery. This is not the place you want to be.
Warning Signs that you may be suffering from Adrenal Fatigue
It is more than just fatigue. Adrenal Fatigue affects a number of hormones, and those hormones can affect almost every part of our body. And so, Adrenal Fatigue tends to present itself differently, in different people. While there are common complaints, there is also a large number of less common symptoms, which is why a proper diagnosis can be difficult to get.
> Morning fatigue - Difficulty getting up in the morning, even after a long sleep.
> Fatigue throughout the day - Without the necessary cortisol output, Adrenal Fatigue can make it difficult to maintain any kind of reasonable energy level throughout the day.
> Difficulty falling asleep - A typical progression after being tired all day is to get an energy boost in the evening, particularly in the early stages of Adrenal Fatigue.
> Cravings - Cravings for salty and sugary foods reflects the bodies inability to balance the levels of minerals in the blood.
> Inability to handle stress - Without sufficient hormones to regulate our stress response, we are unable to increase our physical strength, or mental focus and awareness when needed.
> Weakened immune system - Initially, high levels of cortisol can suppress your immune system and leave you vulnerable to infection. Once progressed, low levels of cortisol associated with Adrenal Fatigue can lead to chronic inflammation, allergies and even autoimmune diseases.
> Digestive complaints - elevated levels of cortisol can cause digestive complaints through inhibiting digestion and reducing levels of good bacteria in the gut (see below).
> Other symptoms often experienced by Adrenal Fatigue sufferers:
- Weight gain
- Decreased libido (sex drive)
- Depression
- Muscle weakness or tension
- Irritability or poor focus (brain fog)
- Hair loss
- Frequent urination
- Extreme tiredness after exercise
So what’s the connection with Adrenal Fatigue and IBS?
The relationship between Adrenal Fatigue and IBS is complex. Basically, IBS has a role to play in the development of Adrenal Fatigue and Adrenal Fatigue has a role to play in the development of IBS… and once you have both, they can just keep making each other worse (6, 7). Firstly the underlying chronic stress caused by IBS (such as a parasite, food sensitivity, bacterial overgrowth, etc.) can lead to eventual Adrenal Fatigue. Secondly, the increased cortisol, adrenaline and other hormones released as a result of stress can, as mentioned above, suppress the immune system, inhibit digestion and even reduce the number of good bacteria in our gut. All of which, can lead to IBS symptoms (6).
So, it’s a little bit chicken and egg, but the key to reversing Adrenal Fatigue is to identify the sources of chronic stress, including those in your gut, and eliminate these. It’s is only once all stress has been removed from the body, that your HPA axis can start to recover and function as it should.
Can I get tested?
Functional Adrenal Stress Profile
For our Australian clients we test for Adrenal Fatigue using the NutriPATH Functional Adrenal Stress Profile. It is a saliva test that evaluates the impact of chronic stress on the body by measuring cortisol and other key hormones; DHEA, eostrogens, progesterone, testosterone and melatonin at four time-points throughout the day.
NutriPATH Functional Adrenal Stress Profile Result - Example Extract for a client with Adrenal Fatigue/exhaustion
There are a few key things we are looking for from this test:
1. Total cortisol output: this measure helps us determine which phase of cortisol dysregulation you are in (homeostasis, acute, compensatory or exhaustion) and whether or not you are suffering from Adrenal Fatigue
2. Daily rhythm: Ever heard of the circadian rhythm? This is a natural rhythm in the body where cortisol is high in the morning to give you lots of energy to get up and start your day, then lowers by the evening as melatonin, your sleep hormone rises and gets you ready for sleep. We like to see a nice rhythm of cortisol production (high in the morning, low at night) throughout the day but there are many factors that can mess with this that we use as clues about your current state of health.
3. Relative elevation in cortisol output at any point throughout the day: These relative elevations give us clues about factors that may be contributing to your overall levels of stress throughout the day. For example, a relative elevation in the morning may be because of your immune system being over-active throughout the night. A elevation at noon or in the afternoon may be from food sensitivities, caffeine, drugs/medicines, allergies, environmental stressors that you came into contact with throughout the day. Finally a relative elevation at night is really interesting to me - they are often caused by immune activity, parasites or some other form of gut infection - a leading cause of IBS
This test is often used as a gateway to further testing because Adrenal Fatigue is not the end point, rather it is a clue that there is an underlying root cause to your symptoms and further investigation is required. At this point, depending on a client’s symptoms and history, I commonly recommend a stool test to check for gut infections, a food sensitivity test to work out which foods are inflammatory to you and a leaky gut test to check out the current state of your gut lining.
If you think this sounds like you, get in touch and we can do some testing to figure out what is going on for you: CLICK HERE
How do I reverse Adrenal Fatigue
Successfully healing Adrenal Fatigue requires a holistic approach focussed on fixing the root cause of your problems and supporting your body through the healing process. This means we are going beyond just temporary symptom relief. We want you to return to vibrant health so you can get back to the active and healthy lifestyle that Adrenal Fatigue is holding you back from. Again, we would be completing further testing to get to the root cause of your issues, but this protocol is a great starting point for healing. We focus on five essential areas for fast and long-term healing.
Diet
The first step is to remove foods that are causing artificial stimulation and inflammation. Here is a list of the main things to consider:
> The stimulants - sugar, caffeine and alcohol. All three lead to the release of more cortisol and act like a further stressor on the body (4, 8, 9).
> The top 5 known inflammatory foods are a good place to start for lowering inflammation in your body; gluten, dairy, soy, corn and eggs should be removed first.
> Food sensitivities identified via testing that are specific to you. Food sensitivities are like little bombs that go off in your gut and cause damage every time you eat them. They must be removed for a minimum of three months to give your gut space to heal, lower inflammation and reduce the burden on your adrenals.
So what can you eat? Simple! Just eat real food - JERF. Like, fruits, vegetables, grains, nuts, seeds, oils, meat, poultry and fish. And focus on the following.
> Good quality fats from coconut, olive oil and organic meats.
> Green leafy vegetables like spinach, kale and chard.
> Seaweed, because of its high iodine content (hello sushi!)
Rest
Rest is an essential component of any healing protocol and often overlooked. Know this: if you don’t give your body the rest it needs to heal, you will not get better. Ideally, go to bed before 10pm. 7-8 hours sleep each night is an absolute must. Did you know that physical repair of the body happens from 10pm to around 2am? Good “sleep hygiene” means turning off those screens (phone, laptop and TV) and allowing one hour before sleep each evening to wind-down by reading a book, journaling, meditating or listen to relaxing music. Trust me, this practice alone will change your quality of sleep if you commit.
Exercise
Too much or too intense exercise for those with Adrenal Fatigue can put added stress on the body and do more harm than good (10). While it’s always important to move your body, a more gentle approach, with exercise such as walking, yoga and restorative pilates will likely have the most positive impact on your healing (11). Once the fatigue has gone, you can return to all of the crazy-active things you love. Read more about this HERE.
Stress Reduction
Removing and reducing stress on the body is a crucial part of any Adrenal Fatigue healing protocol. This applies to all three categories of stress:
> Mental/emotional: implementing relaxation and stress reduction activities such as meditation or acupuncture.
> Physical: consider working with a chiropractor or other health professional to address any structural problems adding to your body’s overall stress.
> Hidden/internal: these are things like hormone imbalances, liver issues, food sensitivities, leaky gut or pathogens that we need to test for and eliminate to stop the constant inflammation in your body. I can help you with this.
Supplementation
Through my study I have learnt that it is almost impossible to obtain all of the necessary nutrients we need for healing from our food alone. A pretty shocking truth and why we need to be smart and supplement (12). A few of my go-to supplements that support the adrenals include:
> Adrenal adaptogens - These are a blend of herbs and roots that support the adrenal glands. Blends commonly include ashwagandha, ginseng, licorice root, holy basil, schisandra and rhodiola. If you are looking for a product to try, aim for something that contains a few of these and take it in the mornings.
> Adrenal glandulars - These are most commonly created from bovine adrenal glands that are dried and desiccated. They can be used as an alternative to the adaptogens or in addition to them. As with the adaptogens, take these in the morning and it is likely you will not need to supplement further with B vitamins.
> B Vitamins - I looove B vitamins. They are awesome first thing in the morning to help with boosting your energy for the day, and those of you who are suffering from Adrenal Fatigue are highly likely to be deficient in B’s. Bioavailability of Vitamin B can be problematic, so I like to use liposomal liquid blends that are absorbed via the mucosal lining of the mouth, rather than in capsule form via the gut
> Magnesium - This mineral helps the body fight off adrenal insufficiency so you can supplement, use a magnesium spray or enjoy a good old Epsom salt bath.
If you are interested in getting tested for Adrenal Fatigue and having a personalised healing protocol developed specifically for you, please head to the Work With Us page to learn more about how we work online with clients in many countries to test for and treat the many root causes of Adrenal Fatigue, IBS symptoms and other GI conditions.
References:
Salleh, M. R. (2008). Life Event, Stress and Illness. The Malaysian Journal of Medical Sciences : MJMS, 15(4), 9–18 LINK
Smith, S. M., & Vale, W. W. (2006). The role of the hypothalamic-pituitary-adrenal axis in neuroendocrine responses to stress. Dialogues in Clinical Neuroscience, 8(4), 383–395 LINK
McEwen, B. S. (2005). Stressed or stressed out: What is the difference? Journal of Psychiatry and Neuroscience, 30(5), 315–318 LINK
Stephens, M. A. C., & Wand, G. (2012). Stress and the HPA Axis: Role of Glucocorticoids in Alcohol Dependence. Alcohol Research : Current Reviews, 34(4), 468–483 LINK
Hannibal, K. E., & Bishop, M. D. (2014). Chronic Stress, Cortisol Dysfunction, and Pain: A Psychoneuroendocrine Rationale for Stress Management in Pain Rehabilitation. Physical Therapy, 94(12), 1816–1825 LINK
Kennedy, P., et al. (2014). Irritable bowel syndrome: A microbiome-gut-brain axis disorder? World Journal of Gastroenterology : WJG, 20(39), 14105–14125 LINK
Chang, L., et al. (2009). Dysregulation of the hypothalamic-pituitary-adrenal (HPA) axis in irritable bowel syndrome. Neurogastroenterology and Motility : The Official Journal of the European Gastrointestinal Motility Society, 21(2), 149–159 LINK
Lovallo, W. R., Farag, N. H., Vincent, A. S., Thomas, T. L., & Wilson, M. F. (2006). Cortisol responses to mental stress, exercise, and meals following caffeine intake in men and women. Pharmacology, Biochemistry, and Behavior, 83(3), 441–447 LINK
9.Gonzalez-Bono, E., et al. (2002). Glucose but not protein or fat load amplifies the cortisol response to psychosocial stress. Horm Behav, 41(3), 328-33 LINK
Brooks, K., & Carter, J. (2013). Overtraining, Exercise, and Adrenal Insufficiency. Journal of Novel Physiotherapies, 3(125), 11717 LINK
Arora, S., & Bhattacharjee, J. (2008). Modulation of immune responses in stress by Yoga. International Journal of Yoga, 1(2), 45–55 LINK
Head, K., Kelly, G. (2009). Nutrients and botanicals for treatment of stress: Adrenal Fatigue, neurotransmitter imbalance, anxiety, and restless sleep. Altern Med Rev, 14(2), 114-40 LINK